Individualised Medicine for Viral Infections

Research focus
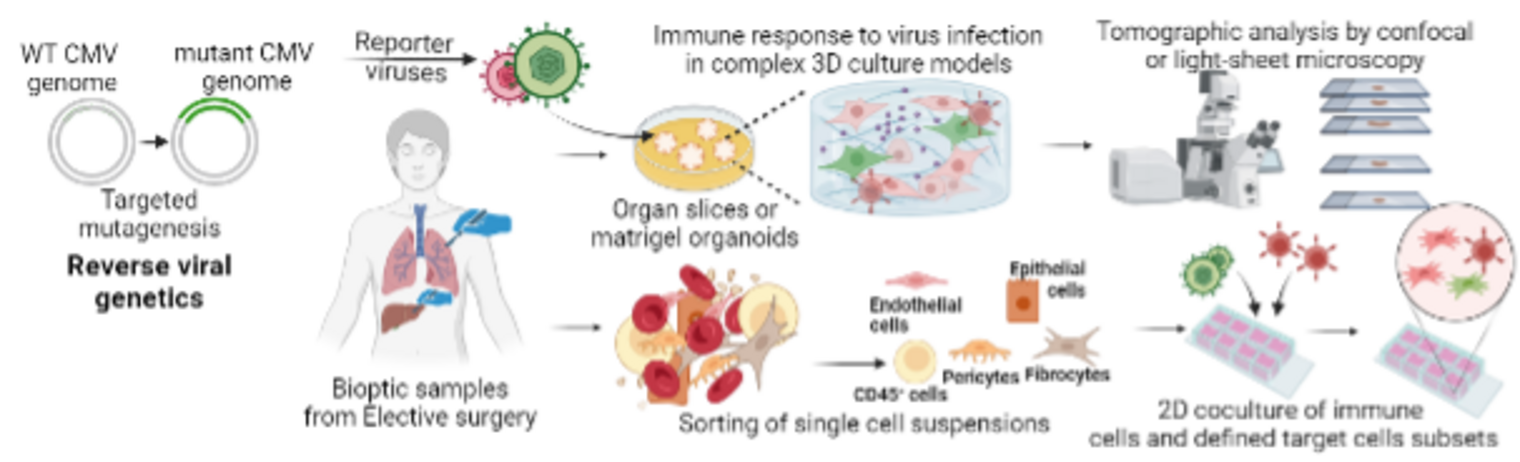
Our research focuses on the analysis of the immune response to viral infections, with a strong focus on clinically relevant infection, such as the Cytomegalovirus (CMV) or Severe Acute respiratory Distress Coronavirus 2 (SARS-CoV-2). CMV is the most common congenital infectious cause and a widespread opportunistic pathogen that latently persists in most people worldwide. Virus reactivation typically occurs in individuals with weakened immune systems, whether due to illness, immunosuppression after organ transplantation, or older individuals with age-related immune weakening. We aim to identify the cellular reservoirs of CMV latency, identify immune mechanisms preventing virus reactivation and determine optimal antigenic targets for adoptive T-cell immunotherapy.
Research focus
Our research focuses on the analysis of the immune response to viral infections, with a strong focus on clinically relevant infection, such as the Cytomegalovirus (CMV) or Severe Acute respiratory Distress Coronavirus 2 (SARS-CoV-2). CMV is the most common congenital infectious cause and a widespread opportunistic pathogen that latently persists in most people worldwide. Virus reactivation typically occurs in individuals with weakened immune systems, whether due to illness, immunosuppression after organ transplantation, or older individuals with age-related immune weakening. We aim to identify the cellular reservoirs of CMV latency, identify immune mechanisms preventing virus reactivation and determine optimal antigenic targets for adoptive T-cell immunotherapy.
Our other focus is to identify serological correlates of immune protection against COVID, to expedite developments and clinical monitoring of future universal and non-waning COVID vaccines.
Prof Dr Luka Cicin-Sain
Viral Immunology is a highly translational branch of science, at the interface of cutting edge biological discoveries and clinical needs of the general population and especially the vulnerable populations. Working on these important topics at CIIM is an earnest responsibility and a distinguished privilege.

Born in Croatia, Luka Cicin-Sain studied medicine at the University of Rijeka, his hometown. In 1996, he earned a degree as MD, started his clinical internship and a master program in biomedicine. He passed the Croatian state exam for physicians and finished his master program in 2004. Meanwhile he worked at the Department of Histology and Embryology in Rijeka and at the Max von Pettenkofer Institute for Hygiene and Medical Microbiology in Munich and attained a PhD degree in 2006. He moved as a postdoctoral fellow of the German Scientific Foundation (DFG) to the Vaccine and Gene Therapy Institute of the Oregon Health and Science University in Portland, USA, where he subsequently became a research assistant professor. In 2010, he returned to Germany as to lead the junior research group "Immune Aging and Chronic Infections" at HZI. In 2016 he was tenured, in 2020 he became the speaker of the HZI Research Topic Immune Responses and Immune Interventions and in 2021 he became the chairperson of the Department "Viral Immunology" (VIRI) at the same institute. In 2020, he cofounded the work group Vaccines of the German Immunological Society, where he is still a co-coordinator.
Running projects
- CMV latency and reactivation in lung transplantation, funded by DZIF and the RESIST excellence cluster flexible funds, in collaboration with Danny Jonigk and Jan C. Kamp.
Publications: Kasmapour B, et al. et Čičin-Šain L. 2018 Myeloid dendritic cells repress human cytomegalovirus gene expression and spread by releasing interferon-unrelated soluble antiviral factors J Virol. 92(1). pii: e01138-17. - T-cell immunotherapy of opportunistic CMV infections in transplantations, funded by DZIF TTU 07.835 and in collaboration with D. Busch, T. Käuferle, B. Eiz-Vesper and A. Moosmann.
Publications: Chaudhry MZ, et al et Čičin-Šain L. Cytomegalovirus Inhibition of Extrinsic Apoptosis Determines Fitness and Resistance to Cytotoxic CD8 T Cells PNAS 117(23):12961-12968.
Khan F, et al. et Cicin-Sain L. Dynamic monitoring of viral gene expression reveals rapid antiviral effects of CD8 T cells recognizing the HCMV-pp65 antigen. bioRxiv. 2023:2023.07.11.548645. doi: 10.1101/2023.07.11.548645 - Neutralization capacity as correlate of anti-COVID immune protection, funded by COFONI in collaboration with S. Pöhlmann, S. Dübel, A. Protic, M. Pavletic and M. Lerga
Publications: Schubert M, et al et Čičin-Šain L, Hust M. 2022 Human serum from SARS-CoV-2 vaccinated and COVID-19 patients shows reduced binding to the RBD of SARS-CoV-2 Omicron variant BMC Medicine doi: 10.1186/s12916-022-02312-5
Kučan-Brlić P, Pavletić M, et al. et Čičin-Šain L. 2022 SARS-CoV-2 Spike and Nucleocapsid Antibody Response in Vaccinated Croatian Healthcare Workers and Infected Hospitalized Patients: A Single Center Cohort Study, Viruses 14(9):1966; doi: 10.3390/v14091966. Jacobsen H, et al et Cicin-Sain L. 2022 Diminished neutralization responses towards SARS-CoV-2 Omicron VoC after mRNA or vector-based COVID-19 vaccinations, Sci Reports; 12(1):19858. doi: 10.1038/s41598-022-22552-y.
Team
The current team list can be found on the group's page on the HZI website.
Further information
The group of „Viral Immunology“ welcomes applications from qualified candidates for PhD or PostDoc positions at any time. Additionally, we continuously offer Master/Bachelor research projects. If you are interested, please contact Prof. Dr. Dr. Luka Cicin-Sain or Claudia Munzel.